The role of imaging in the diagnosis of lung cancer in primary care (PhD)
Start Date Mar 2018
Code L1-C, PhD
Status Ongoing
Collaborators: Pete Wheatstone (PPI)
Introduction
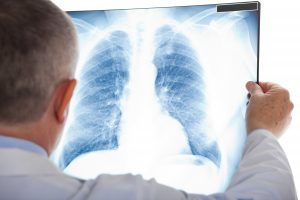 Lung cancer is a leading cause of death worldwide. In the UK survival for patients diagnosed with lung cancer has been worse than for patients in many countries in Europe and North America. An important reason for this is that patients in the UK tend to be diagnosed when their cancer is more advanced, rather than at earlier stages of the disease.
Lung cancer is a leading cause of death worldwide. In the UK survival for patients diagnosed with lung cancer has been worse than for patients in many countries in Europe and North America. An important reason for this is that patients in the UK tend to be diagnosed when their cancer is more advanced, rather than at earlier stages of the disease.
Chest x-ray is a test that is widely used by GPs to diagnose lung cancer. In some patients who have lung cancer, this will not be identified on their chest x-ray – a ‘false negative’ result. We do not know in exactly how many patients chest x-ray does not identify possible cancer, or if missing lung cancer on a chest x-ray causes harm in terms of delayed diagnosis or cancer being more advanced.
Aims & objectives
- Establish how accurate chest x-ray is in diagnosing lung cancer
- Work out the risk of having lung cancer with a normal chest x-ray result, when a patient has certain symptoms
- Find out if patients who are diagnosed with lung cancer and who are registered with GP practices that organise more chest x-rays are diagnosed at earlier stages of lung cancer
Methodology
The first part of the PhD is a systematic review which will collate the available evidence for the accuracy of chest x-ray in identifying lung cancer.
Two studies will be undertaken using routinely collected data. The first of these will examine the accuracy of chest x-ray in a large patient group and examine if patients who have lung cancer, which is not identified on chest x-ray, have worse outcomes. The second study will use data to work out the risk of lung cancer in patients with particular symptoms when the chest x-ray is normal.
A final study will use data from the national cancer registry and the diagnostic imaging dataset to work out if varying rates of chest x-ray by GPs affects the stage at which lung cancer is diagnosed.
Outputs & impact
We expect to publish the results of these studies in a series of papers. The first study (a systematic review on the sensitivity of chest x-ray for diagnosis of lung cancer) will be published in the British Journal of General Practice in October 2019.
This research will produce greater understanding as to the accuracy of chest x-ray and could inform national policy on the role of chest x-ray in lung cancer diagnosis. It may also be useful in contributing to health economic work on the costs and benefits associated with using chest x-ray compared to other tests like low dose CT.
Next steps
The necessary ethical permissions have been obtained for most of the projects. The two studies using routinely collected data will begin in Winter 2019 and will conclude in Summer or Autumn 2020.
The final study, which will use national cancer registry data will require the collation of data from multiple sources, which will be undertaken from December 2019, with an expectation that the study should be completed by January 2022.
Publications
- Bradley SH, Kennedy MPT, Neal R. Recognising Lung Cancer in Primary Care. Advances in Therapy, 2018, 36 (1):19-30, doi: 10.1007/s12325-018-0843-5
- Bradley SH, Abraham S, Callister M, Grice A, Hamilton W, Rodriguez Lopez R, Shinkin B, Neal R. Sensitivity of chest x-ray for detecting lung cancer in people presenting with symptoms: systematic review. British Journal of General Practice, 2019, doi: 10.3399/bjgp19X706853
- Bradley SH, Hatton NLF, Aslam R, Bhartia B, Callister MEJ, Kennedy MPT, Mounce L, Shinkins B, Hamilton WT, Neal RD. Estimating lung cancer risk from chest x-ray and symptoms: a prospective cohort study. British Journal of General Practice, 2020, doi: 10.3399/bjgp20X713993
- Bradley SH, Shinkins B, Kennedy MP. What is the balance of benefits and harms for lung cancer screening with low-dose computed tomography? Journal of the Royal Society of Medicine, 2021, 114(4):164-170. doi: 10.1177/0141076821991108
- Bhartia B.S.K, Hatton N, Aslam R, Bradley SH, Darby M, Hamilton W, Hurst E, Kennedy M.P.T, Mounce L.T.A., Neal R.D., Shinkins B, Callister M.E.J. A prospective cohort evaluation of the sensitivity and specificity of the chest X-ray for the detection of lung cancer in symptomatic adults. European Journal of Radiology, 2021, doi.org/10.1016/j.ejrad.2021.109953.
- Bradley SH, Bhartia BS, Callister ME, Hamilton WT, Hatton NLF, Kennedy MP, Mounce L, Shinkins B, Neal R, et al. Chest X-ray sensitivity and lung cancer outcomes: a retrospective observational study. British Journal of General Practice, 2021. doi: 10.3399/BJGP.2020.1099
- Bradley SH, Bhartia BS, Kennedy MP, Frank LK, Watson J. Investigating suspected lung cancer. BMJ 2022; 378 :e068384 doi: 10.1136/bmj-2021-068384
- Bradley SH, Barclay M, Cornwell B, Abel GA, Callister MEJ, Gomez-Cano M, Round T, Shinkins B, Neal RD. Associations between general practice characteristics and chest X-ray rate: An observational study. British Journal of General Practice 2022; 72 (714): e34-e42. doi: 10.3399/BJGP.2021.0232


