Multi-parametric magnetic resonance imaging (mpMRI) for prostate cancer diagnosis in primary care (PhD)
Start Date Feb 2018
Code E4-C, PhD
Status Ongoing
Collaborators: Dr Steph Archer (Cambridge), Prof Hashim Ahmed (Imperial College Healthcare)
Introduction
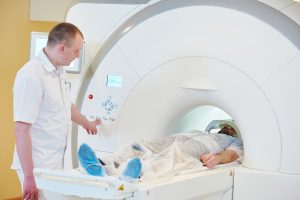 Prostate cancer is the most common type of cancer in men worldwide, and whilst many men can live for years after being diagnosed, it still causes a significant number of deaths. Diagnosing prostate cancer at an early stage is important to reduce a man’s risk of dying from the disease, but tests currently used to diagnose prostate cancer are sometimes inaccurate and can cause significant side effects for patients.
Prostate cancer is the most common type of cancer in men worldwide, and whilst many men can live for years after being diagnosed, it still causes a significant number of deaths. Diagnosing prostate cancer at an early stage is important to reduce a man’s risk of dying from the disease, but tests currently used to diagnose prostate cancer are sometimes inaccurate and can cause significant side effects for patients.
Magnetic resonance imaging (MRI) scans of the pelvis could potentially be used to investigate men with symptoms that might indicate they have prostate cancer. Recent studies have suggested that MRI scans may be accurate enough to decide whether or not such men would need to undergo a procedure to take a biopsy of the prostate to confirm they have cancer. These studies have all been conducted with men who have been referred to hospital, and it is not yet known what impact these MRI scans could have for patients in primary care.
Aim
To examine whether magnetic resonance imaging (MRI) can be utilised in primary care to improve prostate cancer diagnosis
Objectives
- Critically appraise existing evidence for improved patient outcomes and cost effectiveness of MRI as a diagnostic test for prostate cancer
- Understand the acceptability of MRI as a diagnostic test for prostate cancer amongst medical professionals and patients
- Evaluate the cost-effectiveness of direct access MRI testing for symptomatic primary care patients with possible prostate cancer
- Develop possible new primary care diagnostic pathways to incorporate MRI for patients with possible prostate cancer
Methodology
This project will utilise a number of methodologies to explore whether it would be safe, acceptable, and cost effective for GPs to order MRI scans for men with symptoms suggesting a possible diagnosis of prostate cancer. Systematic reviews will examine the evidence that already exists relating to the cost effectiveness and patient outcomes of MRI scanning for men with possible prostate cancer.
A qualitative interview study with healthcare professionals and patients will seek to understand their knowledge and attitudes towards using MRI scans to diagnose prostate cancer. Cost effectiveness analysis using a Markov model with data from recent trials of MRI scans in prostate cancer and NHS costing data will produce estimates as to whether using MRI scans in primary care would be cost-effective.
Outputs & impact
It is anticipated that this project will generate at least 3-4 publications in high impact, peer-reviewed, academic journals to share the key findings from the studies. The health economic modelling could potentially inform future policy and clinical guideline decisions around the application of mpMRI in the diagnostic pathway for prostate cancer in the NHS.
If this project finds mpMRI to be safe, acceptable and cost effective as a diagnostic test for prostate cancer, it could form the basis for further work piloting its use in primary care as a direct access diagnostic test. This pilot work could lead to a full cluster randomised trial.
Next steps
Work on this project is already well underway. The systematic review regarding patient centred outcomes associated with diagnostic tests for prostate cancer has commenced. Ethical approval is being sought for the qualitative interview study of patients and healthcare professionals.
Publications
- Merriel SWD, Martins T, Bailey SER. Exploring the Causes of Death Among Patients With Metastatic Prostate Cancer – A Changing Landscape. JAMA Network Open, 4(8):e2120889
- Merriel SWD, Hardy V, Thompson M, Walter FM, Hamilton W. Patient-centered outcomes from multiparametric magnetic resonance imaging (mpMRI) and MRI-guided biopsy for prostate cancer: A systematic review. Journal of the American College of Radiology, 2019, S1546-1440(19)31032-4
- Elwenspoek MMC, Sheppard AL, McInnes MDF, Merriel SWD, Rowe EWJ, Bryant RJ, Donovan JL, Whiting P. Comparison of multiparametric magnet resonance imaging and targeted biopsy with systematic biopsy alone for the diagnosis of prostate cancer: A systematic review and meta-analysis. JAMA Network Open, 2019, 2(8):e198427
- Merriel SWD, Moon, D; Dunde, P; Corcoran, N; Carroll, P; Partin, A; Smith, J A; Hamdy, F; Moore, C; Ost, P; Costello, T. A modified Delphi study to develop a practical guide for selecting patients with prostate cancer for Active Surveillance. BMC Urology, 2021; 21:18, doi: 10.1186/s12894-021-00789-5
- Merriel SWD, Ingle SM, May MT, Martin RM. Retrospective cohort study evaluating clinical, biochemical and pharmacological prognostic factors for prostate cancer progression using primary care data. BMJ Open, 2021;11:e044420. doi: 10.1136/bmjopen-2020-044420
- Merriel SWD, Pocock L, Gilbert E, Creavin S, Walter FM, Spencer A, Hamilton W. Systematic review and meta-analysis of the diagnostic accuracy of prostate-specific antigen (PSA) for the detection of prostate cancer in symptomatic patients. BMC Med 20, 54 (2022). doi: 10.1186/s12916-021-02230-y
- Merriel SWD, Archer S, Forster AS, Eldred-Evans D, McGrath J, Ahmed HU, Hamilton W, Walter FM. Experiences of ‘traditional’ and ‘one-stop’ MRI-based prostate cancer diagnostic pathways in England: a qualitative study with patients and GPs. BMJ Open 2022; 12:e054045. doi: 10.1136/bmjopen-2021-054045


