Examining the evidence for introducing dermoscopy into general practice
CanTest Researcher Dr Owain Jones at the University of Cambridge outlines his recently published work on the use of dermoscopy in general practice to improve the early diagnosis of melanoma.
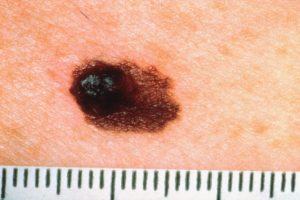 Melanoma is a type of skin cancer: it is currently the 5th commonest cancer in the UK and accounts for 90% of skin cancer deaths. In the UK, most patients with moles they are worried about first go to see their GP, where the GP faces the challenge of distinguishing a rare possible skin cancer from common benign conditions. A dermatoscope is a hand held magnification device and light source that allows clinicians to see deeper under the skin surface – this is known as dermoscopy. Dermoscopy has been shown to improve the accuracy of specialists when diagnosing melanoma and there is now interest in whether it could also be used routinely by GPs. We have recently published two papers reporting findings from studies examining the evidence for introducing dermatoscopy into general practice.
Melanoma is a type of skin cancer: it is currently the 5th commonest cancer in the UK and accounts for 90% of skin cancer deaths. In the UK, most patients with moles they are worried about first go to see their GP, where the GP faces the challenge of distinguishing a rare possible skin cancer from common benign conditions. A dermatoscope is a hand held magnification device and light source that allows clinicians to see deeper under the skin surface – this is known as dermoscopy. Dermoscopy has been shown to improve the accuracy of specialists when diagnosing melanoma and there is now interest in whether it could also be used routinely by GPs. We have recently published two papers reporting findings from studies examining the evidence for introducing dermatoscopy into general practice.
The first study was a survey of UK GPs with a special interest in skin diseases. We found that 97% of the responding GPs were already using dermatoscopes regularly when examining suspicious moles, and 82% felt confident with these skills. An important finding was that 20% of the GPs had not refreshed their dermatoscope training in the last 5 years, highlighting the need for research into the best way for GPs to update their dermoscopy skills and how often they need to do this.
The second study reviewed the current research about the safety and accuracy of dermoscopy when used by GPs. We included 23 studies in our systematic review, although most were undertaken via specialist clinics in hospitals rather than exclusively in the primary care setting. We found some evidence that dermoscopy 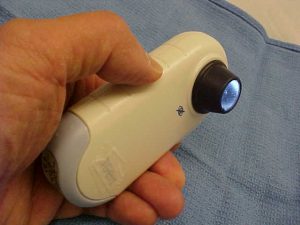 improves the accuracy of GPs when assessing suspicious moles, with a decrease in unnecessary surgery to remove moles and in unnecessary referrals to hospital specialists. However, we also found a number of factors which could stop GPs using dermatoscopes including their cost and the time needed for both training and to use them in clinic.
improves the accuracy of GPs when assessing suspicious moles, with a decrease in unnecessary surgery to remove moles and in unnecessary referrals to hospital specialists. However, we also found a number of factors which could stop GPs using dermatoscopes including their cost and the time needed for both training and to use them in clinic.
Overall, our research has shown that that GPs may be trained to use dermatoscopes routinely and there is some evidence that it will help GPs to assess suspicious moles. However, more evidence is needed from general practice-based research before dermoscopy can be recommended for routine use in primary care. Specifically, we need more evidence around patient views, the most cost-effective approaches and how best to train and maintain GPs skills in dermoscopy.
Find out more about Dr Jones and his CanTest research on his profile page.


