Imaging activity possibly signalling missed diagnostic opportunities in bladder and kidney cancer: a longitudinal data-linkage study using primary care electronic health records
Dr Yin Zhou shares insights from her new paper on how imaging activity can possibly signal missed diagnostic opportunities in bladder and kidney cancer in Cancer Epidemiology.
 Patterns of events before the diagnosis of cancer may reveal ‘signals’ for missed diagnostic opportunities for patients. Earlier research, including from our CanTest collaborators in Denmark, has shown that increase in background rate of consultations, prescriptions and laboratory test use occur long before cancer diagnosis. Imaging tests could be another type of pre-diagnostic feature of potential relevance, but this has not been yet studied in UK patients. Using a novel linked dataset consisting of data from primary care (Clinical Practice Research Datalink), hospital care (HES Diagnostic Imaging Dataset) and the Cancer Registry, we examined patterns of pre-diagnostic imaging test use in bladder and kidney cancer patients diagnosed between 2012-2015 in England.
Patterns of events before the diagnosis of cancer may reveal ‘signals’ for missed diagnostic opportunities for patients. Earlier research, including from our CanTest collaborators in Denmark, has shown that increase in background rate of consultations, prescriptions and laboratory test use occur long before cancer diagnosis. Imaging tests could be another type of pre-diagnostic feature of potential relevance, but this has not been yet studied in UK patients. Using a novel linked dataset consisting of data from primary care (Clinical Practice Research Datalink), hospital care (HES Diagnostic Imaging Dataset) and the Cancer Registry, we examined patterns of pre-diagnostic imaging test use in bladder and kidney cancer patients diagnosed between 2012-2015 in England.
Our study builds on the concept that an ‘early’ imaging test (occurring 4-8 months pre-diagnosis) might represent a missed opportunity to expedite cancer diagnosis. We therefore examined factors associated with a first imaging test occurring 4-8 months pre-diagnosis.
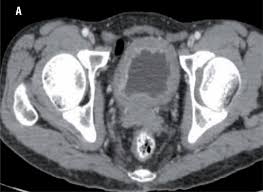 We found that as many as 1 in 5 patients with kidney and bladder cancer had a first imaging test 4-8 months pre-diagnosis. Patients subsequently found to have kidney (but not bladder) cancer, those whose first test was an abdominal X-ray (rather than CT or ultrasound), and those in whom the test was requested by their GP (compared with specialist-requested tests) had a greater probability of having an ‘early’ imaging test. Patients who did not have haematuria before the imaging test was requested also had a greater risk of having a first imaging test 4-8 months pre-diagnosis.
We found that as many as 1 in 5 patients with kidney and bladder cancer had a first imaging test 4-8 months pre-diagnosis. Patients subsequently found to have kidney (but not bladder) cancer, those whose first test was an abdominal X-ray (rather than CT or ultrasound), and those in whom the test was requested by their GP (compared with specialist-requested tests) had a greater probability of having an ‘early’ imaging test. Patients who did not have haematuria before the imaging test was requested also had a greater risk of having a first imaging test 4-8 months pre-diagnosis.
This study uses a novel linked dataset consisting of primary care and cancer registry data, and for the first time added to these data, information on NHS imaging tests. Patients with kidney cancer (which is ‘harder-to-suspect’ than bladder cancer), and without alarm symptoms such as haematuria, would have the greatest potential for faster diagnosis if it was possible to address the potential missed diagnostic opportunities indicated by findings from this study. Our study provides proof of concept that missed diagnostic opportunities relating to the use of imaging tests may exist in some patients subsequently found to have urological cancer.


